1. Hoenders, Velthuis, Vollbehr, Bruggeman, Knegtering, de Jong “Natural Medicines for Psychotic Disorders” US National Library of Medicine and the Journal of Nervous and Mental Disease [INTERNET] 2018 Feb [cited 2022 June 27]
2. Tan MS, Yu JT, Tan CC, Wang HF, Meng XF, Wang C, Jiang T, Zhu XC, Tan L. Efficacy and adverse effects of ginkgo biloba for cognitive impairment and dementia: a systematic review and meta-analysis. J Alzheimers Dis. 2015;43(2):589-603. doi: 10.3233/JAD-140837. PMID: 25114079. [cited 2022 June 27]
3. Genuis S, “Toxic Causes of Mental Illness are Overlooked” Neurotoxicology Journal 2008 Nov [Internet] PMID 18621076 [cited 2022 June 27]
4. Yeager A, “Gut Microbes May Play a Role in Mental Health Disorders” The Scientist [INTERNET] 2019 Jul 5 [cited 2022 June 27]
5. Hills RD Jr, Pontefract BA, Mishcon HR, Black CA, Sutton SC, Theberge CR. Gut Microbiome: Profound Implications for Diet and Disease. Nutrients. 2019 Jul 16;11(7):1613. doi: 10.3390/nu11071613. PMID: 31315227; PMCID: PMC6682904. [cited 2022 June 27]
6. Huang S, Hu H, Sánchez BN, Peterson KE, Ettinger AS, Lamadrid-Figueroa H, Schnaas L, Mercado-García A, Wright RO, Basu N, Cantonwine DE, Hernández-Avila M, Téllez-Rojo MM. Childhood Blood Lead Levels and Symptoms of Attention Deficit Hyperactivity Disorder (ADHD): A Cross-Sectional Study of Mexican Children. Environ Health Perspect. 2016 Jun;124(6):868-74. doi: 10.1289/ehp.1510067. Epub 2015 Dec 8. PMID: 26645203; PMCID: PMC4892926. [cited 2022 June 27]
7. Kennedy C, Yard E, Dignam T, Buchanan S, Condon S, Brown MJ, Raymond J, Rogers HS, Sarisky J, de Castro R, Arias I, Breysse P. Blood Lead Levels Among Children Aged <6 Years – Flint, Michigan, 2013-2016. MMWR Morb Mortal Wkly Rep. 2016 Jul 1;65(25):650-4. doi: 10.15585/mmwr.mm6525e1. PMID: 27359350. [cited 2022 June 27]
8. Al Osman M, Yang F, Massey IY. Exposure routes and health effects of heavy metals on children. Biometals. 2019 Aug;32(4):563-573. doi: 10.1007/s10534-019-00193-5. Epub 2019 Apr 2. PMID: 30941546. [cited 2022 June 27]
9. Orisakwe OE. The role of lead and cadmium in psychiatry. N Am J Med Sci. 2014;6(8):370-376. doi:10.4103/1947-2714.139283 [cited 2022 June 27]
10. Chang CY, Ke DS, Chen JY. Essential fatty acids and human brain. Acta Neurol Taiwan. 2009 Dec;18(4):231-41. PMID: 20329590. [cited 2022 June 27]
11. Stiemsma LT, Nakamura RE, Nguyen JG, Michels KB. Does Consumption of Fermented Foods Modify the Human Gut Microbiota? J Nutr. 2020 Jul 1;150(7):1680-1692. doi: 10.1093/jn/nxaa077. PMID: 32232406; PMCID: PMC7330458. [cited 2022 June 27]
12. Aslam H, Green J, Jacka FN, Collier F, Berk M, Pasco J, Dawson SL. Fermented foods, the gut and mental health: a mechanistic overview with implications for depression and anxiety. Nutr Neurosci. 2020 Sep;23(9):659-671. doi: 10.1080/1028415X.2018.1544332. Epub 2018 Nov 11. PMID: 30415609. [cited 2022 June 27]
13. Hemarajata P, Versalovic J. Effects of probiotics on gut microbiota: mechanisms of intestinal immunomodulation and neuromodulation. Therap Adv Gastroenterol. 2013;6(1):39-51. doi:10.1177/1756283X12459294 [cited 2022 June 27]
14. Szmulewicz A, Samamé C, Caravotta P, et al. Behavioral and emotional adverse events of drugs frequently used in the treatment of bipolar disorders: clinical and theoretical implications. Int J Bipolar Disord. 2016;4(1):6. doi:10.1186/s40345-016-0047-3 [cited 2022 June 27]
15. Nurenberg JR, Schleifer SJ, Shaffer TM, Yellin M, Desai PJ, Amin R, Bouchard A, Montalvo C. Animal-assisted therapy with chronic psychiatric inpatients: equine-assisted psychotherapy and aggressive behavior. Psychiatr Serv. 2015 Jan 1;66(1):80-6. doi: 10.1176/appi.ps.201300524. Epub 2014 Oct 31. PMID: 25269512. [cited 2022 June 27]
16. Lachance L, Ramsey D. Food, mood, and brain health: implications for the modern clinician. Mo Med. 2015 Mar-Apr;112(2):111-5. PMID: 25958655; PMCID: PMC6170050. [cited 2022 June 27]
17. Ergün C, Urhan M, Ayer A. A review on the relationship between gluten and schizophrenia: Is gluten the cause? Nutr Neurosci. 2018 Sep;21(7):455-466. doi: 10.1080/1028415X.2017.1313569. Epub 2017 Apr 9. PMID: 28393621. [cited 2022 June 27]
18. Roopram SM, Burger AM, van Dijk DA, Enterman J, Haffmans J. A pilot study of bright light therapy in schizophrenia. Psychiatry Res. 2016 Nov 30;245:317-320. doi: 10.1016/j.psychres.2016.07.034. Epub 2016 Jul 19. PMID: 27568303. [cited 2022 June 27]
19. Sarris J. Herbal medicines in the treatment of psychiatric disorders: 10-year updated review. Phytother Res. 2018 Jul;32(7):1147-1162. doi: 10.1002/ptr.6055. Epub 2018 Mar 25. PMID: 29575228. [cited 2022 June 27]
20. Sarris J, Panossian A, Schweitzer I, Stough C, Scholey A. Herbal medicine for depression, anxiety and insomnia: a review of psychopharmacology and clinical evidence. Eur Neuropsychopharmacol. 2011 Dec;21(12):841-60. doi: 10.1016/j.euroneuro.2011.04.002. Epub 2011 May 23. PMID: 21601431. [cited 2022 June 27]
21. Alexiuk NA, Vriend JP. Melatonin reduces dopamine content in the neurointermediate lobe of male Syrian hamsters. Brain Res Bull. 1993;32(4):433-6. doi: 10.1016/0361-9230(93)90211-s. PMID: 8221133. [cited 2022 June 27]
22. Girdler SJ, Confino JE, Woesner ME. Exercise as a Treatment for Schizophrenia: A Review. Psychopharmacol Bull. 2019 Feb 15;49(1):56-69. PMID: 30858639; PMCID: PMC6386427.[cited 2022 June 27]
23. Broderick P, Benjamin AB. Caffeine and psychiatric symptoms: a review. J Okla State Med Assoc. 2004 Dec;97(12):538-42. PMID: 15732884. [cited 2022 June 27]
24. Wang HR, Woo YS, Bahk WM. Caffeine-induced psychiatric manifestations: a review. Int Clin Psychopharmacol. 2015 Jul;30(4):179-82. doi: 10.1097/YIC.0000000000000076. PMID: 25856116. [cited 2022 June 27]
25. Aucoin M, Bhardwaj S. Generalized Anxiety Disorder and Hypoglycemia Symptoms Improved with Diet Modification. Case Rep Psychiatry. 2016;2016:7165425. doi: 10.1155/2016/7165425. Epub 2016 Jul 14. PMID: 27493821; PMCID: PMC4963565. [cited 2022 June 27]
26. Irish LA, Kline CE, Gunn HE, Buysse DJ, Hall MH. The role of sleep hygiene in promoting public health: A review of empirical evidence. Sleep Med Rev. 2015 Aug;22:23-36. doi: 10.1016/j.smrv.2014.10.001. Epub 2014 Oct 16. PMID: 25454674; PMCID: PMC4400203. [cited 2022 June 27]
27. Kern R S, Glynn S M, Horan W P, Marder S R, Psychosocial Treatments to Promote Functional Recovery in Schizophrenia, Journal of Psychoses and Related Disorders, Schizophrenia Bulletin Vol 35, Issue 2, March 2009, pages 347-361 [cited 2022 June 27]
28. Hasan A, von Keller R, Friemel CM, Hall W, Schneider M, Koethe D, Leweke FM, Strube W, Hoch E. Cannabis use and psychosis: a review of reviews. Eur Arch Psychiatry Clin Neurosci. 2020 Jun;270(4):403-412. doi: 10.1007/s00406-019-01068-z. Epub 2019 Sep 28. PMID: 31563981. [cited 2022 June 27]
29. Fact Sheet: Mental Health and Environmental Exposures, from the Learning and Developmental Disabilities Initiative, published Dec 2006 [cited 2022 June 27]
30. Tsuruga K, Sugawara N, Sato Y, Saito M, Furukori H, Nakagami T, Nakamura K, Takahashi I, Nakaji S, Yasui-Furukori N. Dietary patterns and schizophrenia: a comparison with healthy controls. Neuropsychiatr Dis Treat. 2015 Apr 22;11:1115-20. doi: 10.2147/NDT.S74760. PMID: 25960655; PMCID: PMC4411018. [cited 2022 June 27]
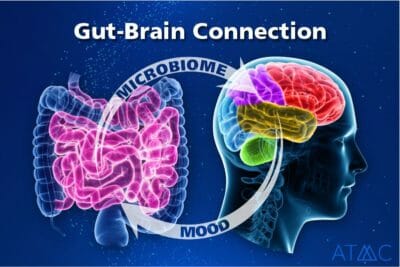 Certain gut bacteria can negatively impact mental health quite dramatically, as studies show.4,5 This is a relatively new branch of research but researchers are finding that the overabundance of certain gut microbes/bacteria shows an observable link to schizophrenia, psychosis, depression, and other mental disorders. This knowledge is gaining much interest to diagnosticians and thankfully, this trend is gaining a more prominent place in the mainstream.
Certain gut bacteria can negatively impact mental health quite dramatically, as studies show.4,5 This is a relatively new branch of research but researchers are finding that the overabundance of certain gut microbes/bacteria shows an observable link to schizophrenia, psychosis, depression, and other mental disorders. This knowledge is gaining much interest to diagnosticians and thankfully, this trend is gaining a more prominent place in the mainstream.
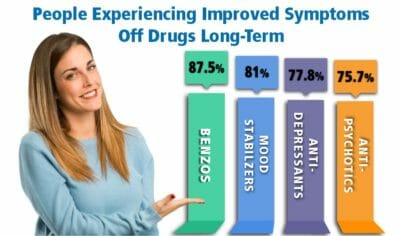
 Alternative to Meds Center is designed to help those in recovery from neuroleptic medications. Drug-based treatments may not have been able to provide the level of relief and wellness that was hoped for over the long term.
Alternative to Meds Center is designed to help those in recovery from neuroleptic medications. Drug-based treatments may not have been able to provide the level of relief and wellness that was hoped for over the long term.








