1. Lakhan SE, Vieira KF. Nutritional and herbal supplements for anxiety and anxiety-related disorders: systematic review. Nutr J. 2010 Oct 7;9:42. doi: 10.1186/1475-2891-9-42. PMID: 20929532; PMCID: PMC2959081. [cited 2022 June 28]
2. Ree E, Redman T, et al., “The Beyond Benzodiazepines Manual.” Reconexxion [Internet] 1997, rev 2010 [cited 2022 June 28]
3. Yang B, Wei J, Ju P, Chen J. Effects of regulating intestinal microbiota on anxiety symptoms: A systematic review. Gen Psychiatr. 2019 May 17;32(2):e100056. doi: 10.1136/gpsych-2019-100056. PMID: 31179435; PMCID: PMC6551444. [cited 2022 June 28]
4. Carpenter JK, Andrews LA, Witcraft SM, Powers MB, Smits JAJ, Hofmann SG. Cognitive behavioral therapy for anxiety and related disorders: A meta-analysis of randomized placebo-controlled trials. Depress Anxiety. 2018 Jun;35(6):502-514. doi: 10.1002/da.22728. Epub 2018 Feb 16. PMID: 29451967; PMCID: PMC5992015. [cited 2022 June 28]
5. Mayo-Wilson E, et al., “Psychological and pharmacological interventions for social anxiety disorder in adults: a systematic review and network meta-analysis” The Lancet Psychiatry, 2014 Sep 25 [Internet] DOI: https://doi.org/10.1016/S2215-0366(14)70329-3 [cited 2022 June 28]
6. Bremner JD, Moazzami K, Wittbrodt MT, Nye JA, Lima BB, Gillespie CF, Rapaport MH, Pearce BD, Shah AJ, Vaccarino V. Diet, Stress and Mental Health. Nutrients. 2020 Aug 13;12(8):2428. doi: 10.3390/nu12082428. PMID: 32823562; PMCID: PMC7468813. [cited 2022 June 28]
7. CDC report Sources of Lead Exposure [published 2022] [cited 2022 June 28]
8. Greenberg, M. I. (2001). Benzodiazepine Withdrawal: Potentially Fatal, Commonly Missed: Following benzodiazepine cessation, withdrawal symptoms may begin within 24 hours or take up to two weeks to develop. Emergency Medicine News, 23(12), 18. [cited 2022 June 28]
9. Ashton H. Protracted withdrawal syndromes from benzodiazepines. J Subst Abuse Treat. 1991;8(1-2):19-28. doi: 10.1016/0740-5472(91)90023-4. PMID: 1675688. [cited 2022 June 28]
10. Overdose Death Rates National Institute on Drug Abuse Mar 10, 2020 [cited 2022 June 28]
11. American Journal of Public Health Increasing Benzodiazepine Prescriptions and Overdose Mortality in the United States, 1996–2013 by Marcus A. Bachhuber MD, MSHP, Sean Hennessy PharmD, PhD, Chinazo O. Cunningham MD, MS, and Joanna L. Starrels MD, MS Published Online: March 09, 2016 [cited 2022 June 28]
12. Ashton H. Guidelines for the rational use of benzodiazepines. When and what to use. Drugs. 1994 Jul;48(1):25-40. doi: 10.2165/00003495-199448010-00004. PMID: 7525193. [cited 2022 June 28]
13. Medical News Today The benefits and risks of benzodiazepines Medically reviewed by Alan Carter, Pharm.D. — Written by Joseph Nordqvist — Updated on November 8, 2020 [cited 2022 June 28]
14. Benzodiazepines: Revisiting Clinical Issues in Treating Anxiety Disorders. Prim Care Companion J Clin Psychiatry. 2005;7(1):23-32. PMID: 15841190; PMCID: PMC1076447.[cited 2022 June 28]
15. Meier PJ, Ziegler WH, Neftel K. Benzodiazepine–Praxis und Probleme ihrer Anwendung [Benzodiazepine–practice and problems of its use]. Schweiz Med Wochenschr. 1988 Mar 19;118(11):381-92. German. PMID: 3287602. [cited 2022 June 28]
16. Otte C. Cognitive behavioral therapy in anxiety disorders: current state of the evidence. Dialogues Clin Neurosci. 2011;13(4):413-421. doi:10.31887/DCNS.2011.13.4/cotte [cited 2022 June 28]
17. American Academy of Sleep Medicine Healthy Sleep Habits Updated Feb. 9, 2017 [cited 2022 June 28]
18. Downie LE, Keller PR, Busija L, Lawrenson JG, Hull CC. Blue‐light filtering spectacle lenses for visual performance, sleep, and macular health in adults. Cochrane Database Syst Rev. 2019;2019(1):CD013244. Published 2019 Jan 16. doi:10.1002/14651858.CD013244 [cited 2022 June 28]
19. Mold Warriors: Fighting America’s Hidden Health Threat Paperback – April 1, 2005 by Ritchie C. Shoemaker (Author), James Schaller (Author), Patti Schmidt (Author) [cited 2022 June 28]
20. Rea WJ, Didriksen N, Simon TR, Pan Y, Fenyves EJ, Griffiths B. Effects of toxic exposure to molds and mycotoxins in building-related illnesses. Arch Environ Health. 2003 Jul;58(7):399-405. doi: 10.1080/00039896.2003.11879140. PMID: 15143852. [cited 2022 June 28]
21. Edmondson DA, Nordness ME, Zacharisen MC, Kurup VP, Fink JN. Allergy and “toxic mold syndrome”. Ann Allergy Asthma Immunol. 2005 Feb;94(2):234-9. doi: 10.1016/S1081-1206(10)61301-4. PMID: 15765738. [cited 2022 June 28]
22. Potera C. Molding a link to depression. Environ Health Perspect. 2007;115(11):A536. doi:10.1289/ehp.115-a536a. [cited 2022 June 28]
23. Miladinovic T, Nashed MG, Singh G. Overview of Glutamatergic Dysregulation in Central Pathologies. Biomolecules. 2015;5(4):3112-3141. Published 2015 Nov 11. doi:10.3390/biom5043112. [cited 2022 June 28]
24. Firth J, Gangwisch JE, Borisini A, Wootton RE, Mayer EA. Food and mood: how do diet and nutrition affect mental wellbeing? [published correction appears in BMJ. 2020 Nov 9;371:m4269]. BMJ. 2020;369:m2382. Published 2020 Jun 29. doi:10.1136/bmj.m2382 [cited 2022 June 28]
25. Orisakwe OE. The role of lead and cadmium in psychiatry. N Am J Med Sci. 2014;6(8):370-376. doi:10.4103/1947-2714.139283. [cited 2022 June 28]
26. Maximino C, Araujo J, Leão LK, Grisolia AB, Oliveira KR, Lima MG, Batista Ede J, Crespo-López ME, Gouveia A Jr, Herculano AM. Possible role of serotoninergic system in the neurobehavioral impairment induced by acute methylmercury exposure in zebrafish (Danio rerio). Neurotoxicol Teratol. 2011 Nov-Dec;33(6):727-34. doi: 10.1016/j.ntt.2011.08.006. Epub 2011 Aug 18. PMID: 21871955. [cited 2022 June 28]
27. Nicholas J. Heyer, Diana Echeverria, Alvah C. Bittner, Jr., Federico M. Farin, Claire C. Garabedian, James S. Woods, Chronic Low-Level Mercury Exposure, BDNF Polymorphism, and Associations with Self-Reported Symptoms and Mood, Toxicological Sciences, Volume 81, Issue 2, October 2004, Pages 354–363. [cited 2022 June 28]
28. Sherman KJ, Ludman EJ, Cook AJ, Hawkes RJ, Roy-Byrne PP, Bentley S, Brooks MZ, Cherkin DC. Effectiveness of therapeutic massage for generalized anxiety disorder: a randomized controlled trial. Depress Anxiety. 2010 May;27(5):441-50. doi: 10.1002/da.20671. PMID: 20186971; PMCID: PMC2922919. [cited 2022 June 28]
29. Aung SK, Fay H, Hobbs RF 3rd. Traditional Chinese Medicine as a Basis for Treating Psychiatric Disorders: A Review of Theory with Illustrative Cases. Med Acupunct. 2013;25(6):398-406. doi:10.1089/acu.2013.1007. [cited 2022 June 28]
30. Pilkington K, Kirkwood G, Rampes H, Cummings M, Richardson J. Acupuncture for anxiety and anxiety disorders–a systematic literature review. Acupunct Med. 2007 Jun;25(1-2):1-10. doi: 10.1136/aim.25.1-2.1. PMID: 17641561. [cited 2022 June 28]
31. Akhondzadeh S, Naghavi HR, Vazirian M, Shayeganpour A, Rashidi H, Khani M. Passionflower in the treatment of generalized anxiety: a pilot double-blind randomized controlled trial with oxazepam. J Clin Pharm Ther. 2001 Oct;26(5):363-7. doi: 10.1046/j.1365-2710.2001.00367.x. PMID: 11679026. [cited 2022 June 28]
32. Savage KM, Stough CK, Byrne GJ, et al. Kava for the treatment of generalised anxiety disorder (K-GAD): study protocol for a randomised controlled trial. Trials. 2015;16:493. Published 2015 Nov 2. doi:10.1186/s13063-015-0986-5. [cited 2022 June 28]
33. Hepsomali P, Groeger JA, Nishihira J, Scholey A. Effects of Oral Gamma-Aminobutyric Acid (GABA) Administration on Stress and Sleep in Humans: A Systematic Review. Front Neurosci. 2020;14:923. Published 2020 Sep 17. doi:10.3389/fnins.2020.00923. [cited 2022 June 28]
34. Jakaria M, Azam S, Haque ME, et al. Taurine and its analogs in neurological disorders: Focus on therapeutic potential and molecular mechanisms. Redox Biol. 2019;24:101223. doi:10.1016/j.redox.2019.101223. [cited 2022 Mar 10] [cited 2022 June 28]
35. Mori M, Gähwiler BH, Gerber U. Beta-alanine and taurine as endogenous agonists at glycine receptors in rat hippocampus in vitro. J Physiol. 2002;539(Pt 1):191-200. doi:10.1113/jphysiol.2001.013147. [cited 2022 June 28]
36. Cleveland WL, DeLaPaz RL, Fawwaz RA, Challop RS. High-dose glycine treatment of refractory obsessive-compulsive disorder and body dysmorphic disorder in a 5-year period. Neural Plast. 2009;2009:768398. doi:10.1155/2009/768398. [cited 2022 June 28]
37. Hospital News Nutritional treatments to combat anxiety disorders 2005-10-01. 2021 [cited 2022 June 28]
38. Smriga M, Ando T, Akutsu M, Furukawa Y, Miwa K, Morinaga Y. Oral treatment with L-lysine and L-arginine reduces anxiety and basal cortisol levels in healthy humans. Biomed Res. 2007 Apr;28(2):85-90. doi: 10.2220/biomedres.28.85. PMID: 17510493. [cited 2022 June 28]
39. Boyle NB, Lawton C, Dye L. The Effects of Magnesium Supplementation on Subjective Anxiety and Stress-A Systematic Review. Nutrients. 2017;9(5):429. Published 2017 Apr 26. doi:10.3390/nu9050429. [cited 2022 June 28]
40. Blessing EM, Steenkamp MM, Manzanares J, Marmar CR. Cannabidiol as a Potential Treatment for Anxiety Disorders.Neurotherapeutics. 2015;12(4):825-836. doi:10.1007/s13311-015-0387-1. [cited 2022 June 28]
41. Garzón, C., Guerrero, J.M., Aramburu, O. et al. Effect of melatonin administration on sleep, behavioral disorders and hypnotic drug discontinuation in the elderly: a randomized, double-blind, placebo-controlled study. Aging Clin Exp Res, 38–42 (2009). https://doi.org/10.1007/BF03324897. [cited 2022 June 28]
42. Zang DX. [A self body double blind clinical study of L-tryptophan and placebo in treated neurosis]. Zhonghua Shen Jing Jing Shen Ke Za Zhi. 1991 Apr;24(2):77-80, 123-4. Chinese. PMID: 1860385. [cited 2022 June 28]
43. Kahn RS, Westenberg HG, Verhoeven WM, Gispen-de Wied CC, Kamerbeek WD. Effect of a serotonin precursor and uptake inhibitor in anxiety disorders; a double-blind comparison of 5-hydroxytryptophan, clomipramine and placebo. Int Clin Psychopharmacol. 1987 Jan;2(1):33-45. doi: 10.1097/00004850-198701000-00003. PMID: 3312397. [cited 2022 June 28]
44. Satoh H. Occupational and environmental toxicology of mercury and its compounds. Ind Health. 2000 Apr;38(2):153-64. doi: 10.2486/indhealth.38.153. PMID: 10812838. [cited 2022 June 28]
45. Birdsall TC. 5-Hydroxytryptophan: a clinically-effective serotonin precursor. Altern Med Rev. 1998 Aug;3(4):271-80. PMID: 9727088. [cited 2022 June 28]
46. Acute Hypoglycemia Presenting as Acute Psychosis Tanveer Padder MD, Aparna Udyawar MD, Nouman Azhar MD, Kamil Jaghab MD From the Department of Psychiatry, Nassau University Medical Center. December 2005. [cited 2022 June 28]
47. Brady WJ Jr, Duncan CW. Hypoglycemia masquerading as acute psychosis and acute cocaine intoxication. Am J Emerg Med. 1999 May;17(3):318-9. doi: 10.1016/s0735-6757(99)90140-7. PMID: 10337905. [cited 2022 June 28]
48. Center for Disease Control and Prevention Nerve Agent and Organophosphate Pesticide Poisoning. [cited 2022 June 28]
49. Organophosphate Toxicity StatPearls Publishing; 2020 Jan-. Erika L. Robb; Mari B. Baker. [cited 2022 June 28]
50. Choudhary AK, Lee YY. Neurophysiological symptoms and aspartame: What is the connection? Nutr Neurosci. 2018 Jun;21(5):306-316. doi: 10.1080/1028415X.2017.1288340. Epub 2017 Feb 15. PMID: 28198207. [cited 2022 June 28]
51. 13 Ingredients to Avoid in Personal Care Products by Meghan Telpner Last updated on July 22nd, 2020. [cited 2022 June 28]
52. Environmental Working Group Report: Organic Packaged Foods Only ‘Clean’ Option for Consumers Over 2,000 Chemicals – Many Toxic – Allowed in Non-Organic Packaged Food Mar 5, 2019. [cited 2022 June 28]
53. Koff A, “What foods contain MSG?” published in Sharecare [Internet] [cited 2022 June 28]
54. Adham AM, Higashiguchi S, Horie K, Kim M, Hatta H, Yokogoshi H. Relaxation and immunity enhancement effects of gamma-aminobutyric acid (GABA) administration in humans. Biofactors. 2006;26(3):201-8. doi: 10.1002/biof.5520260305. PMID: 16971751. [cited 2022 June 28]
55. Fortney L, Taylor M. Meditation in medical practice: a review of the evidence and practice. Prim Care. 2010 Mar;37(1):81-90. doi: 10.1016/j.pop.2009.09.004. PMID: 20188999. [cited 2022 June 28]
56. Natural Mental Health Calm Yourself: Balancing Excess Glutamate and GABA Deficiencies with Supplements & Herbs (part 2) by Henry Emmons, MD Jun 30, 2020 [cited 2022 June 28]
57. Son HK, So WY, Kim M. Effects of Aromatherapy Combined with Music Therapy on Anxiety, Stress, and Fundamental Nursing Skills in Nursing Students: A Randomized Controlled Trial. Int J Environ Res Public Health. 2019;16(21):4185. Published 2019 Oct 29. doi:10.3390/ijerph16214185 [cited 2022 June 28]
58. O’Donnell CP, Allott KA, Murphy BP, Yuen HP, Proffitt TM, Papas A, Moral J, Pham T, O’Regan MK, Phassouliotis C, Simpson R, McGorry PD. Adjunctive Taurine in First-Episode Psychosis: A Phase 2, Double-Blind, Randomized, Placebo-Controlled Study. J Clin Psychiatry. 2016 Dec;77(12):e1610-e1617. doi: 10.4088/JCP.15m10185. PMID: 27835719. [cited 2022 June 28]
59. Shaw K, Turner J, Del Mar C. Tryptophan and 5-hydroxytryptophan for depression. Cochrane Database Syst Rev. 2002;(1):CD003198. doi: 10.1002/14651858.CD003198. PMID: 11869656. [cited 2022 June 28]
60. Wheatley D. Kava and valerian in the treatment of stress-induced insomnia. Phytother Res. 2001 Sep;15(6):549-51. doi: 10.1002/ptr.840. PMID: 11536390. [cited 2022 June 28]
61. Capezuti E, Sagha Zadeh R, Pain K, Basara A, Jiang NZ, Krieger AC. A systematic review of non-pharmacological interventions to improve nighttime sleep among residents of long-term care settings. BMC Geriatr. 2018;18(1):143. Published 2018 Jun 18. doi:10.1186/s12877-018-0794-3 [cited 2022 June 28]
62. Liang S, Wu X, Jin F. Gut-Brain Psychology: Rethinking Psychology From the Microbiota-Gut-Brain Axis. Front Integr Neurosci. 2018;12:33. Published 2018 Sep 11. doi:10.3389/fnint.2018.00033 [cited 2022 June 28]
63. Butler MI, Mörkl S, Sandhu KV, Cryan JF, Dinan TG. The Gut Microbiome and Mental Health: What Should We Tell Our Patients?: Le microbiote Intestinal et la Santé Mentale : que Devrions-Nous dire à nos Patients? Can J Psychiatry. 2019 Nov;64(11):747-760. doi: 10.1177/0706743719874168. Epub 2019 Sep 17. PMID: 31530002; PMCID: PMC6882070. [cited 2022 June 28]
64. Henry-Unaeze HN. Update on food safety of monosodium l-glutamate (MSG). Pathophysiology. 2017 Dec;24(4):243-249. doi: 10.1016/j.pathophys.2017.08.001. Epub 2017 Sep 18. PMID: 28943112. [cited 2022 June 28]
65. Miladinovic T, Nashed MG, Singh G. Overview of Glutamatergic Dysregulation in Central Pathologies. Biomolecules. 2015;5(4):3112-3141. Published 2015 Nov 11. doi:10.3390/biom5043112 [cited 2022 June 28]
66. Mie A, Andersen HR, Gunnarsson S, et al. Human health implications of organic food and organic agriculture: a comprehensive review. Environ Health. 2017;16(1):111. Published 2017 Oct 27. doi:10.1186/s12940-017-0315-4 [cited 2022 June 28]
67. Choudhary AK, Lee YY. Neurophysiological symptoms and aspartame: What is the connection? Nutr Neurosci. 2018 Jun;21(5):306-316. doi: 10.1080/1028415X.2017.1288340. Epub 2017 Feb 15. PMID: 28198207. [cited 2022 June 28]
68. Olsen A, “Caffeine and Aspartame.” published Feb 25, 2013 in The Watchdog (Bellevue College) [cited 2022 June 28]
69. Kim EJ, Lim SY, Lee HJ, Lee JY, Choi S, Kim SY, Kim JM, Shin IS, Yoon JS, Yang SJ, Kim SW. Low dietary intake of n-3 fatty acids, niacin, folate, and vitamin C in Korean patients with schizophrenia and the development of dietary guidelines for schizophrenia. Nutr Res. 2017 Sep;45:10-18. doi: 10.1016/j.nutres.2017.07.001. Epub 2017 Jul 19. PMID: 29037327. [cited 2022 June 28]
70. Genuis SJ. Toxic causes of mental illness are overlooked. Neurotoxicology. 2008 Nov;29(6):1147-9. doi: 10.1016/j.neuro.2008.06.005. Epub 2008 Jun 24. PMID: 18621076. [cited 2022 June 28]
71. Cho HS, Kim S, Lee SY, Park JA, Kim SJ, Chun HS. Protective effect of the green tea component, L-theanine on environmental toxins-induced neuronal cell death. Neurotoxicology. 2008 Jul;29(4):656-62. doi: 10.1016/j.neuro.2008.03.004. Epub 2008 Mar 20. PMID: 18452993. [cited 2022 June 28]
72. Clapp M, Aurora N, Herrera L, Bhatia M, Wilen E, Wakefield S. Gut microbiota’s effect on mental health: The gut-brain axis. Clin Pract. 2017;7(4):987. Published 2017 Sep 15. doi:10.4081/cp.2017.987 [cited 2022 June 28]
73. National Academies of Sciences, Engineering, and Medicine; Health and Medicine Division; Board on Population Health and Public Health Practice; Committee on the Health Effects of Marijuana: An Evidence Review and Research Agenda. The Health Effects of Cannabis and Cannabinoids: The Current State of Evidence and Recommendations for Research. Washington (DC): National Academies Press (US); 2017 Jan 12. 4, Therapeutic Effects of Cannabis and Cannabinoids. Available from: https://www.ncbi.nlm.nih.gov/books/NBK425767/ [cited 2022 June 28]
74. Demisch K, Bauer J, Georgi K, Demisch L. Treatment of severe chronic insomnia with L-tryptophan: results of a double-blind cross-over study. Pharmacopsychiatry. 1987 Nov;20(6):242-4. doi: 10.1055/s-2007-1017114. PMID: 3432357. [cited 2022 June 28]
75. Donath F, Quispe S, Diefenbach K, Maurer A, Fietze I, Roots I. Critical evaluation of the effect of valerian extract on sleep structure and sleep quality. Pharmacopsychiatry. 2000 Mar;33(2):47-53. doi: 10.1055/s-2000-7972. PMID: 10761819. [cited 2022 June 28]
76. Woelk H, Schläfke S. A multi-center, double-blind, randomised study of the Lavender oil preparation Silexan in comparison to Lorazepam for generalized anxiety disorder. Phytomedicine. 2010 Feb;17(2):94-9. doi: 10.1016/j.phymed.2009.10.006. Epub 2009 Dec 3. PMID: 19962288. [cited 2022 June 28]
77. Carnevale G, Di Viesti V, Zavatti M, Zanoli P. Anxiolytic-like effect of Griffonia simplicifolia Baill. seed extract in rats. Phytomedicine. 2011 Jul 15;18(10):848-51. doi: 10.1016/j.phymed.2011.01.016. Epub 2011 Feb 25. PMID: 21353511. [cited 2022 June 28]
78. Pakseresht S, Boostani H, Sayyah M. Extract of valerian root (Valeriana officinalis L.) vs. placebo in treatment of obsessive-compulsive disorder: a randomized double-blind study. J Complement Integr Med. 2011 Oct 11;8:/j/jcim.2011.8.issue-1/1553-3840.1465/1553-3840.1465.xml. doi: 10.2202/1553-3840.1465. PMID: 22718671. [cited 2022 June 28]
79. Tu CH, MacDonald I, Chen YH. The Effects of Acupuncture on Glutamatergic Neurotransmission in Depression, Anxiety, Schizophrenia, and Alzheimer’s Disease: A Review of the Literature. Front Psychiatry. 2019;10:14. Published 2019 Feb 12. doi:10.3389/fpsyt.2019.00014 [cited 2022 June 28]
80. Lakhan SE, Vieira KF. Nutritional and herbal supplements for anxiety and anxiety-related disorders: systematic review. Nutr J. 2010 Oct 7;9:42. doi: 10.1186/1475-2891-9-42. PMID: 20929532; PMCID: PMC2959081. [cited 2022 June 28]
81. Carter S. Origins of Orthomolecular Medicine. Integr Med (Encinitas). 2019;18(3):76-77. [cited 2022 June 28]
82. Chattu VK, Manzar MD, Kumary S, Burman D, Spence DW, Pandi-Perumal SR. The Global Problem of Insufficient Sleep and Its Serious Public Health Implications. Healthcare (Basel). 2018;7(1):1. Published 2018 Dec 20. doi:10.3390/healthcare7010001 [cited 2022 June 28]
83. SAMHSA Treatment Data Set [cited 2022 June 28]
84. Moritz B, Schmitz AE, Rodrigues ALS, Dafre AL, Cunha MP. The role of vitamin C in stress-related disorders. J Nutr Biochem. 2020 Nov;85:108459. doi: 10.1016/j.jnutbio.2020.108459. Epub 2020 Jul 3. PMID: 32745879. [cited 2022 June 28]
85. Young LM, Pipingas A, White DJ, Gauci S, Scholey A. A Systematic Review and Meta-Analysis of B Vitamin Supplementation on Depressive Symptoms, Anxiety, and Stress: Effects on Healthy and ‘At-Risk’ Individuals. Nutrients. 2019;11(9):2232. Published 2019 Sep 16. doi:10.3390/nu11092232 [cited 2022 June 28]
86. Eid A, Khoja S, AlGhamdi S, Alsufiani H, Alzeben F, Alhejaili N, Tayeb HO, Tarazi FI. Vitamin D supplementation ameliorates severity of generalized anxiety disorder (GAD). Metab Brain Dis. 2019 Dec;34(6):1781-1786. doi: 10.1007/s11011-019-00486-1. Epub 2019 Sep 2. PMID: 31478182. [cited 2022 June 28]
87. González MJ, Miranda-Massari JR, Mora EM, Cruzado NA, Jiménez I, Rosa M, Matos Vera MI, Santiago C, Román-Eyxarch MI, Rodríguez JR, Pérez Cortés C, Riordan NH, Riordan HD, Ricart CM. Integrative medicine: a paradigm shift in medical education and practice. P R Health Sci J. 2000 Dec;19(4):389-92. PMID: 11293891. [cited 2022 June 28]
88. Kaličanin B, Velimirović D. A Study of the Possible Harmful Effects of Cosmetic Beauty Products on Human Health. Biol Trace Elem Res. 2016 Apr;170(2):476-84. doi: 10.1007/s12011-015-0477-2. Epub 2015 Aug 23. PMID: 26296330. [cited 2022 June 28]
89. CDC Study brief #377 – Antidepressant Use Among Adults: United States, 2015-2018 [published online Sept 2020] [cited 2022 June 28]
90. Statista report Skin care products frequency of use by gender [published online 2017] [cited 2022 June 28]
91. Bably M, Arif AA, Post A. Prenatal use of cleaning and scented products and its association with childhood asthma, asthma symptoms, and mental health and developmental comorbidities. J Asthma. 2021 Jan;58(1):46-51. doi: 10.1080/02770903.2019.1656229. Epub 2019 Aug 26. PMID: 31449430. [cited 2022 June 28]
92. CDC report: Cadmium Toxicity: How are People Exposed to Cadmium? [published online 2013] [cited 2022 June 28]
93. Society for the Study of Addiction Professor Malcolm Lader 1936-2020 [cited 2022 June 28]
 Choose foods that are chemical and pesticide-free 66
Choose foods that are chemical and pesticide-free 66 According to Butler et al’s research published in 2019, the trillions of micro-organisms in the gut play incredibly important roles in mental health, with the power of influencing mood positively and reducing anxiety. Anxiety and depression are 2 major reasons a large percentage of North Americans seek psychiatric drugs for symptom relief. The microbiome can be healthy and functioning well with the right support or can be out of balance and unable to fulfill its important functions. Just like an orchestra, where one out-of-tune violin can make the whole works sound awfully sour, the workings of the human body were meant to be a harmonized work of art to dwell in. “Tuning-up” the microbiome weighs in as a superior, natural alternative to Ativan and other prescription drugs.63
According to Butler et al’s research published in 2019, the trillions of micro-organisms in the gut play incredibly important roles in mental health, with the power of influencing mood positively and reducing anxiety. Anxiety and depression are 2 major reasons a large percentage of North Americans seek psychiatric drugs for symptom relief. The microbiome can be healthy and functioning well with the right support or can be out of balance and unable to fulfill its important functions. Just like an orchestra, where one out-of-tune violin can make the whole works sound awfully sour, the workings of the human body were meant to be a harmonized work of art to dwell in. “Tuning-up” the microbiome weighs in as a superior, natural alternative to Ativan and other prescription drugs.63 Toxins are among the known causes of anxiety.72 Orisakwe’s 2014 review of hundreds of clinical trials notes that psychiatric symptoms are more prevalent in urban areas compared to rural areas. A further correlation is made between increased pollution of air, water, etc. in urbanized areas, as a likely culprit for toxic effects. (also see the section on toxic body care products, below.) Over the course of life, toxins accumulate in the cells of the body, the blood, the brain, and the nervous system. These toxins can create the effect of an over-stimulated nervous system. Pesticides are a good example to understand this phenomenon. Pesticides are designed to kill insects, for example, grasshoppers, and function in the following way: the toxin permeates into the exoskeleton and finds its way to the nervous system. Pesticides cause acetylcholine channels to stay open, not allowing these channels to properly close. Acetylcholine is a stimulating neurotransmitter and will make the grasshopper jump, twitch, have muscle contractions, and eventually become exhausted. This continual activation of acetylcholine channels eventually puts the grasshopper into a catatonic state followed by death. This is how pesticides kill pests and their mechanisms of action are similar to the way excitotoxins harm human cells by the overstimulation that occurs after toxic exposures.71
Toxins are among the known causes of anxiety.72 Orisakwe’s 2014 review of hundreds of clinical trials notes that psychiatric symptoms are more prevalent in urban areas compared to rural areas. A further correlation is made between increased pollution of air, water, etc. in urbanized areas, as a likely culprit for toxic effects. (also see the section on toxic body care products, below.) Over the course of life, toxins accumulate in the cells of the body, the blood, the brain, and the nervous system. These toxins can create the effect of an over-stimulated nervous system. Pesticides are a good example to understand this phenomenon. Pesticides are designed to kill insects, for example, grasshoppers, and function in the following way: the toxin permeates into the exoskeleton and finds its way to the nervous system. Pesticides cause acetylcholine channels to stay open, not allowing these channels to properly close. Acetylcholine is a stimulating neurotransmitter and will make the grasshopper jump, twitch, have muscle contractions, and eventually become exhausted. This continual activation of acetylcholine channels eventually puts the grasshopper into a catatonic state followed by death. This is how pesticides kill pests and their mechanisms of action are similar to the way excitotoxins harm human cells by the overstimulation that occurs after toxic exposures.71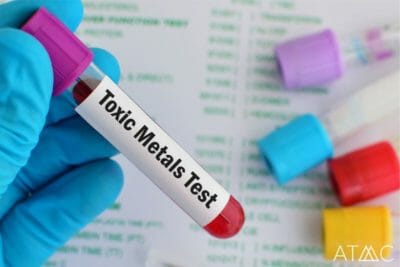 A wealth of research data has documented the adverse effects of heavy metals on the body and on mental health. Heavy metals can include lead from proximity to airplane fuel or older water pipes (pre-1978), mercury, commonly found in dental amalgam, and cadmium from tobacco grown in contaminated soil, as a few examples of sources of potential exposures.7,25,92
A wealth of research data has documented the adverse effects of heavy metals on the body and on mental health. Heavy metals can include lead from proximity to airplane fuel or older water pipes (pre-1978), mercury, commonly found in dental amalgam, and cadmium from tobacco grown in contaminated soil, as a few examples of sources of potential exposures.7,25,92 An article by Shaheen and Vieria was published in The Nutritional Journal in 2010 that reviewed over 60 studies on approximately 2600 participants using nutritional and herbal remedies for treating psychiatric symptoms. Their review concluded that “based on the available evidence, it appears that nutritional and herbal supplementation is an effective method for treating anxiety and anxiety-related conditions without the risk of serious side effects.” 80 Our work using nutritional and other alternatives to Ativan and similar drugs to help our clients at Alternative to Meds Center resonates in full harmony with their findings. This and other studies have found “strong evidence” for the efficacy of numerous alternative treatments including passionflower, kava, and combinations of amino acids such as L-lysine and L-arginine and others, as effective treatments for anxiety and other symptoms.34,35,36,38,31
An article by Shaheen and Vieria was published in The Nutritional Journal in 2010 that reviewed over 60 studies on approximately 2600 participants using nutritional and herbal remedies for treating psychiatric symptoms. Their review concluded that “based on the available evidence, it appears that nutritional and herbal supplementation is an effective method for treating anxiety and anxiety-related conditions without the risk of serious side effects.” 80 Our work using nutritional and other alternatives to Ativan and similar drugs to help our clients at Alternative to Meds Center resonates in full harmony with their findings. This and other studies have found “strong evidence” for the efficacy of numerous alternative treatments including passionflower, kava, and combinations of amino acids such as L-lysine and L-arginine and others, as effective treatments for anxiety and other symptoms.34,35,36,38,31 What really sets us apart from other residential mental health treatment centers is our concentration on the
What really sets us apart from other residential mental health treatment centers is our concentration on the 







