Diet Modification — Strong Support for Natural Mental Health
 According to a massive review in the Nutrients Journal, adequate intake of fruits and vegetables plays an observably therapeutic role in mental health. Another comprehensive literature review published in the Journal of Neuropsychobiology identifies specific nutritional interventions that when lacking, are associated with higher incidences of disorders such as depression, psychosis, and schizophrenia. Backed up by over 600 studies, specific nutrients are documented to have positive effects on mental health.
According to a massive review in the Nutrients Journal, adequate intake of fruits and vegetables plays an observably therapeutic role in mental health. Another comprehensive literature review published in the Journal of Neuropsychobiology identifies specific nutritional interventions that when lacking, are associated with higher incidences of disorders such as depression, psychosis, and schizophrenia. Backed up by over 600 studies, specific nutrients are documented to have positive effects on mental health.
Among those cited are zinc, magnesium, omega-3 fatty acids, selenium, vitamin C, vitamin B6, B12, folate, amino acids, the 9 essential amino acids, and many others as preventative and therapeutic agents that are essential to mental wellness. Excellent choices to add to the daily diet include green leafy vegetables, fresh fruit, Brazil nuts, avocados, chicken, cheese, yogurt, milk, (organic) soy, olive oil, grass-fed beef, other meat products, shrimp, and fatty fish. One study showed that closely following the Mediterranean diet provided a 42% reduction in depression symptoms among 10,000 university students over the 4.5 years the study was conducted. Whole and unprocessed foods provide high nutrient content in a low-carb context. Nutrition can be a powerful alternative to Lybalvi and other medications.7,8,30-32
The Connection Between Gut Health and Mental Wellness
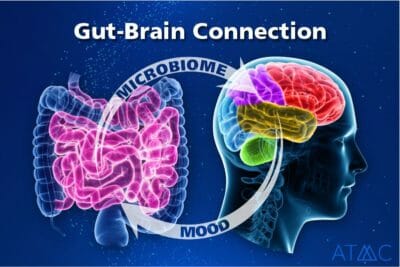 The majority of neurotransmitters are produced and distributed in the gut. This remarkable “mental health machine” requires the proper raw materials to produce adequate and quality natural neurochemicals that support thousands upon thousands of essential functions in the body, including the CNS, and the brain. No drug can produce neurotransmitters. You literally cannot live, or live well, without these chemical messengers. A healthy and functioning microbiome has been studied as a treatment strategy for both preventing and treating disorders such as schizophrenia. Supporting the microbiome is possible through adding fermented foods daily such as yogurt, sauerkraut, and kimchi, as well as plant-sourced fiber and adhering to the Mediterranean diet. Avoiding high-intake of sugar and inflammatory processed food is also protective of essential beneficial microbiota of the gut. Implementing nutrition-based actions can provide excellent choices for alternatives to Lybalvi. 4,6,9,33,34
The majority of neurotransmitters are produced and distributed in the gut. This remarkable “mental health machine” requires the proper raw materials to produce adequate and quality natural neurochemicals that support thousands upon thousands of essential functions in the body, including the CNS, and the brain. No drug can produce neurotransmitters. You literally cannot live, or live well, without these chemical messengers. A healthy and functioning microbiome has been studied as a treatment strategy for both preventing and treating disorders such as schizophrenia. Supporting the microbiome is possible through adding fermented foods daily such as yogurt, sauerkraut, and kimchi, as well as plant-sourced fiber and adhering to the Mediterranean diet. Avoiding high-intake of sugar and inflammatory processed food is also protective of essential beneficial microbiota of the gut. Implementing nutrition-based actions can provide excellent choices for alternatives to Lybalvi. 4,6,9,33,34
Physical Exercise as an Alternative to Lybalvi
A 2018 Danish study published in the Journal of Schizophrenia Research found that of the 428 participants suffering from symptoms of schizophrenia, only one-fifth of the group complied with the recommended 30 minutes of daily exercise. The authors suggested that generally, low activity levels may be a significant contributing factor to the weight gain and “waist gain” that commonly plagues this population.22
 A recently published 2022 report published in the Frontiers in Psychiatry Journal reports on a 12-month study involving daily exercise and a modified diet. All the participants suffered from obesity. Half were on pharmacologic treatments for a mental disorder, and half were cardiac patients, also on pharmaceutical treatments. A control group was also observed who did not participate in the diet interventions or the exercise program. The participants who did the daily exercise and modified diet lost an average of 15 pounds of excess weight. They also scored higher ratings for quality of life, better metabolism, and improved clinical outcomes.4
A recently published 2022 report published in the Frontiers in Psychiatry Journal reports on a 12-month study involving daily exercise and a modified diet. All the participants suffered from obesity. Half were on pharmacologic treatments for a mental disorder, and half were cardiac patients, also on pharmaceutical treatments. A control group was also observed who did not participate in the diet interventions or the exercise program. The participants who did the daily exercise and modified diet lost an average of 15 pounds of excess weight. They also scored higher ratings for quality of life, better metabolism, and improved clinical outcomes.4
Based on these and other studies, daily exercise appears to be a wise alternative to Lybalvi, an antipsychotic drug compounded with an opioid receptor blocker, devised to chemically mitigate weight gain which is a common outcome in persons taking antipsychotic medications. There are other benefits to exercise apart from weight management. Popular therapeutic exercises include Qi Gong and Tai Chi, both of which can have significant positive effects on physical health, as well as improved mental well-being. Speak to your prescribing physician about exercise as a safer alternative to Lybalvi and similar antipsychotic medications.1-3,26,44,45
CBT — Effective Nonpharmacologic Treatment
CBT or cognitive behavioral counseling is well-documented as a beneficial non-drug-based therapy to assist persons suffering from mental health disorders such as depression, bipolar, schizophrenia, and other troubling challenging life issues. Persons can benefit in a wide variety of ways such as reduction of symptoms of psychosis, low mood, and improved cognitive function — but also gain insights and strategies leading to many highly practical improvements such as vocational satisfaction and improved earning ability. With the use of CBT perhaps your goal is to acquire relationship skills, better financial management skills, and find relief from past trauma or from current sources of stress. These and many other changes can be facilitated through personal counseling to improve one’s overall quality of life.10,12,34
Mindfulness and Relaxation Therapies
 The physical benefits of yoga exercises and stretching are well known. Yoga enthusiasts love what this practice can do for muscle flexibility and strength, relief of lower back pain, improved circulation and oxygen levels in the blood, and better posture. But there are also many mental wellness benefits that have been clinically studied, verifying their effectiveness as an alternative to Lybalvi and other medications.
The physical benefits of yoga exercises and stretching are well known. Yoga enthusiasts love what this practice can do for muscle flexibility and strength, relief of lower back pain, improved circulation and oxygen levels in the blood, and better posture. But there are also many mental wellness benefits that have been clinically studied, verifying their effectiveness as an alternative to Lybalvi and other medications.
In a study published in the Primary Care Companion for CNS Disorders, authors Cabral et al found that yoga provides significant positive changes in major psychiatric disorders including schizophrenia and psychosis in a much less toxic way than prescription medicine.35,36
There are many relaxation and mindfulness therapies that have been found very beneficial for persons suffering from lingering mental disorders and symptoms. Some popular examples that can have both physical and mental benefits include mindfulness meditation, Qigong, guided imagery, progressive muscle relaxation, therapeutic massage, Reiki, and breathwork.4,9
Neurotoxin Removal — Benefits to Mental Health
It is not possible to overstate the importance of clearing out toxic accumulations from the body. Neurotoxins are pervasive in the modern world. Coupled with the fact that some persons are more sensitive than others to these invading disruptors, there is ample research now that shows the benefits of cleansing the body of toxic materials such as heavy metals like lead, cadmium, and mercury, as well as chemical exposures that can occur in a work environment, in the home, from processed foods, or contacted in agricultural and outdoor settings. Toxic exposure is probably one of the most overlooked root causes of psychiatric symptoms. Cleaning these out of the body can provide some of the most surprisingly beneficial results for improvements in mood, thoughts, quality of sleep, and behaviors, as well as improved physical well-being.15,17,18,27,39
Specific Nutrients as Lybalvi Alternatives and What to Avoid
Supplements can bridge the gap between what we get from the foods we choose and what the body and CNS actually need for full support. One example is amino acids, which are essential for CNS function, and while the body can create some of these from the foods we eat, a person typically needs supplements for an adequate and complete supply.
Of particular interest for recovery of natural mental health are adequate levels of the B vitamins, vitamin C, vitamin D, omega-3 oils, magnesium, zinc, selenium, and many others, especially where deficiencies are discovered from testing.
 It is recommended to avoid excess sugars, artificial sweeteners, flavor enhancers like MSG, caffeine, and refined carbs. MSG can be found in many processed foods as an additive, under various names like “fortified protein,” “China salt,” or “yeast nutrient.” Some persons are highly sensitive to MSG especially when combined with common elements like vinegar or corn starch or others that can trigger a toxic reaction.46 These food additives can spike blood sugar levels and cause inflammation, negative emotions, and features of psychosis. Better choices would be slow-burning sugars from complex carbs, and foods that are as unprocessed as possible. Choose foods that are clean of chemicals and preservatives and taste enhancers. These food additives can cause neurophysiological symptoms including seizures, depression, anxiety, insomnia, irritable moods, impaired memory, lowered cognitive function, and learning problems. Flavor enhancers and additives are often used in processed food in combination, and as a result, their harmful potential would be significantly worsened.
It is recommended to avoid excess sugars, artificial sweeteners, flavor enhancers like MSG, caffeine, and refined carbs. MSG can be found in many processed foods as an additive, under various names like “fortified protein,” “China salt,” or “yeast nutrient.” Some persons are highly sensitive to MSG especially when combined with common elements like vinegar or corn starch or others that can trigger a toxic reaction.46 These food additives can spike blood sugar levels and cause inflammation, negative emotions, and features of psychosis. Better choices would be slow-burning sugars from complex carbs, and foods that are as unprocessed as possible. Choose foods that are clean of chemicals and preservatives and taste enhancers. These food additives can cause neurophysiological symptoms including seizures, depression, anxiety, insomnia, irritable moods, impaired memory, lowered cognitive function, and learning problems. Flavor enhancers and additives are often used in processed food in combination, and as a result, their harmful potential would be significantly worsened.
Gluten is another element to avoid wherever possible, especially if gluten or wheat, or grain sensitivity has been determined. A massive review of studies has shown the positive effects of a gluten-free diet on symptoms of depression, anxiety, and insomnia and to a lesser degree, cognitive function, schizophrenia, and disorders on the autism spectrum. Foods that are high in gluten include baked goods, pasta, cereals, and even gravy thickeners.48 It is best to avoid such potential health disruptors.
But food doesn’t have to be bland to be health-enhancing. Many herbs and culinary spices can add tantalizing flavors as well as health benefits such as antioxidant anti-inflammatory agents, anticarcinogenic (anti-cancer) properties, support for heart and respiratory health, as well as benefits to cognitive function and mood. Some notable spices include rosemary, sage, oregano, black pepper, chili pepper, turmeric, garlic, ginger, and cinnamon.7,11,29,40,41
The field of herbal pharmacology is receiving much attention as researchers continue to discover benefits for mental wellness. Botanical and phytomedicines such as Hypericum perforatum, Passiflora incanata, Ginkgo biloba, Crocus sativus, and many others have been shown helpful in treating depression, anxiety, and insomnia. While more research is needed, herbal-based medicine is an important asset in the field of holistic treatments.47
Avoid Cannabis and Other Recreational Drugs
Often a person taking antipsychotic medications will become emotionally blunted, and desperate for some stimulation. The person may be drawn towards recreational drug and alcohol use and even overconsume caffeine and energy drinks just for a “lift.” This is a very bad idea. Cannabis is associated with an increased proclivity to psychosis and other unwanted outcomes. Avoid it. Alcohol is another drug to avoid for many reasons. including protecting the volume of the very valuable white matter that makes up the inner part of the brain.19-21, 42,43
Learn More about Lybalvi Alternatives at Alternative to Meds Center
Alternative to Meds Center is a warm and welcoming inpatient facility that lies at the foot of the majestic Red Rocks of Arizona. It is a peaceful, healing, and tranquil setting. Numerous hiking and biking trails are close by. The town of Sedona is nearby, known as an artist’s haven, with many beautiful and colorful experiences to visit and enjoy.
 Over 40 licensed staff and medical doctors provide oversight and guidance in designing the uniquely tailored program that will best enhance each client’s journey back to natural mental health.
Over 40 licensed staff and medical doctors provide oversight and guidance in designing the uniquely tailored program that will best enhance each client’s journey back to natural mental health.
Protocols used in treatment include many holistic therapies and strategies, such as lab testing, holistic cessation, neurotransmitter rehabilitation, Orthomolecular medicine, therapeutic massage and spa services, yoga, acupuncture, cleansing and sauna therapies, IV + NAD treatments, nebulized glutathione, Equine assisted therapy, CBT and other counseling services, Qigong, Peer Support programs and much more. Holistic detox programs are medically supervised, and a rich array of comfort therapies is provided to ease the transition to drug-free safely, gently, and effectively.
Contact us today for more information about our programs and protocols, insurance coverage, or any other questions you may have. We know that in your decision-making phase of selecting a treatment plan, you are searching for a program that best serves your or your loved one’s unique needs and situation. We have helped many thousands of clients achieve their health goals. Our world-class facility and Lybalvi alternatives program may be just what you have been searching for.
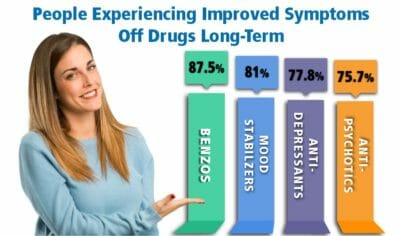
 While weight gain is a significant concern with antipsychotics in general, there are many other concerns associated with antipsychotic medication. While drugs for psychosis, bipolar, and schizophrenia have their place in treatment, many feel long-term use can introduce more negatives than positives.13-14 Antipsychotics generally suppress dopamine, which is like living in a rather dim, emotionless, joyless space. Alternative science-based medicine may help eliminate such problems using effective and safer strategies, allowing a person to feel alive again, but without the symptoms that led to being prescribed a mind-numbing drug in the first place. Once a person has stabilized after a psychotic episode, this may be a good time to consider transitioning to a more satisfactory and appropriate treatment protocol.
While weight gain is a significant concern with antipsychotics in general, there are many other concerns associated with antipsychotic medication. While drugs for psychosis, bipolar, and schizophrenia have their place in treatment, many feel long-term use can introduce more negatives than positives.13-14 Antipsychotics generally suppress dopamine, which is like living in a rather dim, emotionless, joyless space. Alternative science-based medicine may help eliminate such problems using effective and safer strategies, allowing a person to feel alive again, but without the symptoms that led to being prescribed a mind-numbing drug in the first place. Once a person has stabilized after a psychotic episode, this may be a good time to consider transitioning to a more satisfactory and appropriate treatment protocol. According to a massive review in the Nutrients Journal, adequate intake of fruits and vegetables plays an observably therapeutic role in mental health. Another comprehensive literature review published in the Journal of Neuropsychobiology identifies specific nutritional interventions that when lacking, are associated with higher incidences of disorders such as depression, psychosis, and schizophrenia. Backed up by over 600 studies, specific nutrients are documented to have positive effects on mental health.
According to a massive review in the Nutrients Journal, adequate intake of fruits and vegetables plays an observably therapeutic role in mental health. Another comprehensive literature review published in the Journal of Neuropsychobiology identifies specific nutritional interventions that when lacking, are associated with higher incidences of disorders such as depression, psychosis, and schizophrenia. Backed up by over 600 studies, specific nutrients are documented to have positive effects on mental health. The majority of neurotransmitters are produced and distributed in the gut. This remarkable “mental health machine” requires the proper raw materials to produce adequate and quality natural neurochemicals that support thousands upon thousands of essential functions in the body, including the CNS, and the brain. No drug can produce neurotransmitters. You literally cannot live, or live well, without these chemical messengers. A healthy and functioning microbiome has been studied as a treatment strategy for both preventing and treating disorders such as schizophrenia. Supporting the microbiome is possible through adding fermented foods daily such as yogurt, sauerkraut, and kimchi, as well as plant-sourced fiber and adhering to the Mediterranean diet. Avoiding high-intake of sugar and inflammatory processed food is also protective of essential beneficial microbiota of the gut. Implementing nutrition-based actions can provide excellent choices for alternatives to Lybalvi. 4,6,9,33,34
The majority of neurotransmitters are produced and distributed in the gut. This remarkable “mental health machine” requires the proper raw materials to produce adequate and quality natural neurochemicals that support thousands upon thousands of essential functions in the body, including the CNS, and the brain. No drug can produce neurotransmitters. You literally cannot live, or live well, without these chemical messengers. A healthy and functioning microbiome has been studied as a treatment strategy for both preventing and treating disorders such as schizophrenia. Supporting the microbiome is possible through adding fermented foods daily such as yogurt, sauerkraut, and kimchi, as well as plant-sourced fiber and adhering to the Mediterranean diet. Avoiding high-intake of sugar and inflammatory processed food is also protective of essential beneficial microbiota of the gut. Implementing nutrition-based actions can provide excellent choices for alternatives to Lybalvi. 4,6,9,33,34 A recently published 2022 report published in the Frontiers in Psychiatry Journal reports on a 12-month study involving daily exercise and a modified diet. All the participants suffered from obesity. Half were on pharmacologic treatments for a mental disorder, and half were cardiac patients, also on pharmaceutical treatments. A control group was also observed who did not participate in the diet interventions or the exercise program. The participants who did the daily exercise and modified diet lost an average of 15 pounds of excess weight. They also scored higher ratings for quality of life, better metabolism, and improved clinical outcomes.4
A recently published 2022 report published in the Frontiers in Psychiatry Journal reports on a 12-month study involving daily exercise and a modified diet. All the participants suffered from obesity. Half were on pharmacologic treatments for a mental disorder, and half were cardiac patients, also on pharmaceutical treatments. A control group was also observed who did not participate in the diet interventions or the exercise program. The participants who did the daily exercise and modified diet lost an average of 15 pounds of excess weight. They also scored higher ratings for quality of life, better metabolism, and improved clinical outcomes.4 The physical benefits of yoga exercises and stretching are well known. Yoga enthusiasts love what this practice can do for muscle flexibility and strength, relief of lower back pain, improved circulation and oxygen levels in the blood, and better posture. But there are also many mental wellness benefits that have been clinically studied, verifying their effectiveness as an alternative to Lybalvi and other medications.
The physical benefits of yoga exercises and stretching are well known. Yoga enthusiasts love what this practice can do for muscle flexibility and strength, relief of lower back pain, improved circulation and oxygen levels in the blood, and better posture. But there are also many mental wellness benefits that have been clinically studied, verifying their effectiveness as an alternative to Lybalvi and other medications. It is recommended to avoid excess sugars, artificial sweeteners, flavor enhancers like MSG, caffeine, and refined carbs. MSG can be found in many processed foods as an additive, under various names like “fortified protein,” “China salt,” or “yeast nutrient.” Some persons are highly sensitive to MSG especially when combined with common elements like vinegar or corn starch or others that can trigger a toxic reaction.46 These food additives can spike blood sugar levels and cause inflammation, negative emotions, and features of psychosis. Better choices would be slow-burning sugars from complex carbs, and foods that are as unprocessed as possible. Choose foods that are clean of chemicals and preservatives and taste enhancers. These food additives can cause neurophysiological symptoms including seizures, depression, anxiety, insomnia, irritable moods, impaired memory, lowered cognitive function, and learning problems. Flavor enhancers and additives are often used in processed food in combination, and as a result, their harmful potential would be significantly worsened.
It is recommended to avoid excess sugars, artificial sweeteners, flavor enhancers like MSG, caffeine, and refined carbs. MSG can be found in many processed foods as an additive, under various names like “fortified protein,” “China salt,” or “yeast nutrient.” Some persons are highly sensitive to MSG especially when combined with common elements like vinegar or corn starch or others that can trigger a toxic reaction.46 These food additives can spike blood sugar levels and cause inflammation, negative emotions, and features of psychosis. Better choices would be slow-burning sugars from complex carbs, and foods that are as unprocessed as possible. Choose foods that are clean of chemicals and preservatives and taste enhancers. These food additives can cause neurophysiological symptoms including seizures, depression, anxiety, insomnia, irritable moods, impaired memory, lowered cognitive function, and learning problems. Flavor enhancers and additives are often used in processed food in combination, and as a result, their harmful potential would be significantly worsened. Over 40 licensed staff and medical doctors provide oversight and guidance in designing the uniquely tailored program that will best enhance each client’s journey back to natural mental health.
Over 40 licensed staff and medical doctors provide oversight and guidance in designing the uniquely tailored program that will best enhance each client’s journey back to natural mental health.







